pathogenic micro-organisms
Reading time:Unlike the preceding category, these are living organisms that share parasitic properties and that are capable of proliferating in a higher organism (especially humans) by inducing more or less serious health disorders; water, for these micro-organisms, merely constitutes a means of transport and of contamination. They have limited survival capability but a lifetime that varies depending on the organism concerned: the spore-forming or encysted forms are the most resistant; some viruses and bacteria can be hosted by parasite reservoirs; some worms have larvae forms that can develop in one or more intermediate hosts living in an aquatic environment (molluscs, crustaceans or fish). Their persistence also depends on the medium’s physical-chemical conditions, on predators …
Water intended to produce drinking water can contain a wide variety of pathogenic micro-organisms. Consequently, their identification and elimination require different techniques.
Some have only come to light during recent decades, e.g.
- Legionella, Campylobacter, Helicobacter, Mycobacterium and Escherichia coli O157:H7 strain;
- Rotavirus, Calicivirus (Norwalk and hepatitis E), SARS Coronavirus;
- Sporozoa (parasitic protozoa) of the orders Coccidia (Cryptosporidium, Cyclospora, Toxoplasma) or Microsporidia (Enterocytozoon, Encephalitozoon, Nosema…).
There are a number of different reasons for the late discovery of these pathogenic agents, termed "emergent": progress achieved in epidemiological studies and investigation methods, extension of diseases caused by certain technical advances (e.g. legionnaire’s disease and air conditioning systems), increased populations at risk (especially in the case of patients suffering from AIDS), population migration, ecological disturbances; at times, we can be dealing with truly new strains (appearing as the result of mutations, recombinations, plasmid transfer by bacteriophages …) as is probably the case for E. coli O157: H7 whose toxin is very similar to that of the Shigella.
These organisms can be allocated to the following major groups: viruses, bacteria, fungi, protozoa, worms, insects.
viruses
Viruses (figure 11) are extremely small pathogenic agents that are only visible under an electronic microscope and that can only multiply inside a living cell (see section viruses). When such a cell is attacked by a virus, it soon totally transforms into a granular heap of new viruses ready to infect new cells.

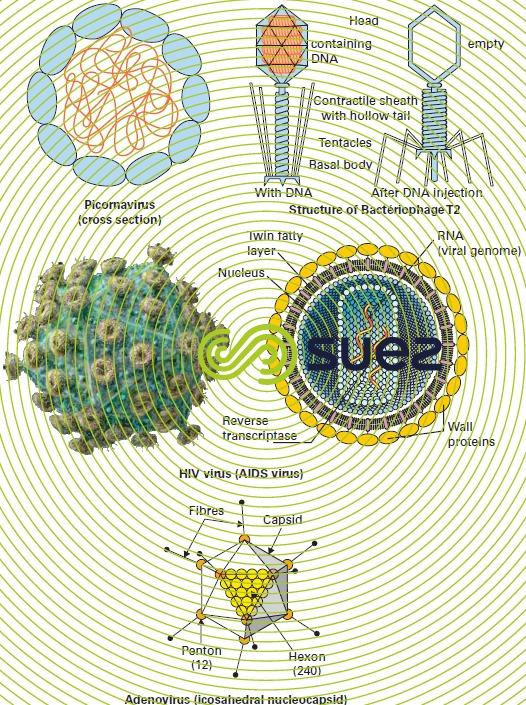

The following viruses can be found in water:
- Enteroviruses: these viruses are part of the picornavirus group ("pico" = very small – " RNA " – "virus"), of which, in all, there are several tens of different types:
- the poliomyelitis virus that attacks nerve centres (paralysis, lymphocytic meningitis);
- ECHO virus (Enteric Cytopathogenic Human Orphan virus), that causes a generally benign intestinal disorder (diarrhoea in children); some serological types can transmit (reversible) lymphocytic meningitis;
- Coxsackie A and B, capable of causing lymphocytic meningitis, respiratory disorders, myalgia or myocardia. These viruses also cause infantile gastro-enteritis;
- Hepatitis A virus: this is the agent of one of the oldest and most frequent waterborne diseases (whereas types B, C and D are transmitted by blood transfusions or by various types of contact between individuals). This disease is endemic in certain hot regions where the virus survives longer in the water than the poliovirus or the echovirus. This virus is also one of the most resistant to chlorine;
- Caliciviruses that particularly include the Norwalk virus (gastro-enteritis) and the hepatitis E virus (presenting a particular danger to pregnant women). Contamination is caused by ingesting dirty water, bathing or eating shellfish;
- Adenoviruses that attack the upper respiratory system and the eyes (a source of conjunctivitis in swimming pools) but arealso present in the intestine;
- Reoviruses responsible for diarrhoea, skin eruptions and disorders of the upper respiratory system;
- Rotaviruses, identified in many cases of gastro-enteritis (e.g. 64 000 cases in Great Britain between 2000 and 2003); livestock is often responsible for contaminating surface water;
- The SARS Coronavirus, deadly pneumopathy that appeared in Asia towards the end of 2002 and that had spread worldwide by 2003; it is an airborne virus; however, the presence of the infectious virus in the urine and faeces of patients showed that waterborne transmission was also possible;
- Influenza that swimming pools can accidentally help to transmit because the virus is very abundant in nasal mucus;
- Papillomavirus, responsible for verrucas contracted in swimming pools.
In fact, the role played by water in the transmission of certain viral illnesses is very controversial. Additionally, if we refer to the rare cases where it has been possible to ascribe viral epidemics to a waterborne source, the water in question had always been massively contaminated by sewage water; however, the minimum doses causing an infection are as yet unknown.
When viruses are present in water, they are usually found in small quantities. Therefore, the water to be analysed first has to be concentrated (see section microbiological analysis).
bacteria
Certain types of bacteria are specifically pathogenic in nature; however, there are germs that are normally non-virulent but that can reveal a degree of pathogenicity in favourable environmental conditions or when, by accident, they are able to penetrate via an unusual biological route (e.g. Escherichia coli in the blood).
After being isolated, bacteria are identified by being regrown on specific media using chemical reagents and/or seroagglutination techniques for highlighting all their biochemical, cytoplasmic or membrane properties as well as their virulence (figures 12 and 13).

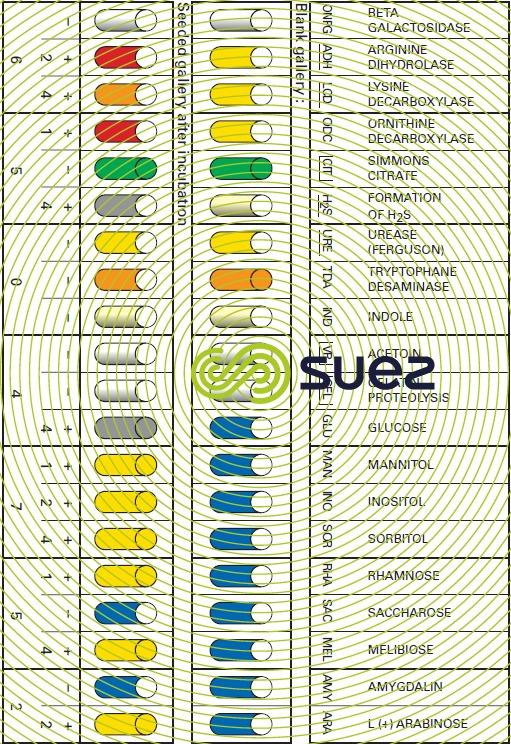


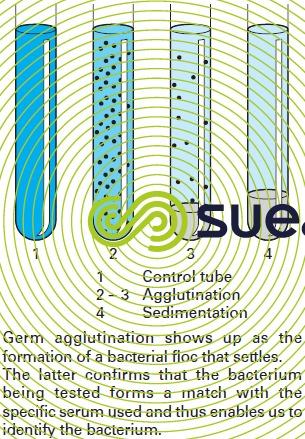

The bacteriological quality of water must be systematically checked with the view to ensuring the absence of any pathogenic germs; this inspection is most frequently carried out using an indirect method that solely checks for the absence of faecal contamination test germs (see section microbiological analysis).
Nevertheless, since Pasteur’s time, specific media and reactions have been developed for the purpose of highlighting the nature and virulence of all pathogenic bacteria. The techniques applied to water are usually derived from those developed for the hospital environment. The additional problem inherent to the aquatic environment is the high level of dilution affecting target germs and also the state of stress sometimes inflicted on them by their stay in water. Their isolation, therefore, calls for special concentration (filter membranes) and regrowth (incubation techniques involving several temperature stages) techniques.
The main pathogenic bacteria emitted to the receiving medium by healthy or diseased carriers and that can be transmitted in water to non-immunised subjects, include:
enterobacteria
- the bacilli responsible for typhoid and paratyphoid fevers:
- the typhus bacillus or Eberth's bacillus; Salmonella typhi;
- Salmonella paratyphi A and B, respectively Salmonella paratyphi and S. schottmuelleri.
- bacilli responsible for dysentery such as:
- Shigella dysenteriae and Sh. paradysenteriae;
- Shigella flexneri or the Flexner bacillus (pseudo dysenteric, endemic form of the disease). Gastro-intestinal disorders that include the salmonellosis (e.g. Salmonellaenterica) and the shigellosis, have not all been clearly characterised: there are numerous benign cases;
- Escherichia coli (common name: colibacillus) responsible for colibacillosis; in fact, there are various strains of this bacillus and some are harmless (E.coli forms part of the intestinal flora and is the main faecal contamination test-germ) while others are pathogenic and cause dysentery (one of the causes of « traveller’s diarrhoea»), urinary infections and neonatal meningitis. The 0157:H7strain recently detected is particularly virulent (fatalities in the USA, Canada, Scotland …); this bacillus fixes onto the intestinal wall and, while inducing bloody diarrhoea, it secretes a toxin responsible for causing haemorrhaging; this toxin is carried in the blood and capable of causing irreversible damage to the kidneys, the intestine, the pancreas and the brain.
vibrio organisms
- The vibrio responsible for cholera (Vibrio cholerae or V. comma),discovered by Koch and present in the form of small flagellate and motile arched rods. Cholera epidemics are still fairly frequent and inadequate disinfection of drinking water constitutes one of the main causes of this disease in third world countries;
- Aeromonas hydrophila: gastro-enteritis and diarrhoea.
spirilla organisms
- Campylobacter (C. jejuni, C. coli) which, having been regarded as mainly part of animal pathology, now represents a cause of human enteritis that is just as important as the salmonellas or E. coli O157:H7;
- Helicobacter pylori: gastro-enteritis, ulcers and cancers of the digestive tract.
pseudomonadaceae
- the pyocyanic bacillus (Pseudomonas aeruginosa) frequently found in sewer water and also the Ps. Fluorescens cause diarrhoea.
parvobacteriaceae
- Pasteurella (or Francisella) tularensis causing tularemia, a disease that is usually transmitted from one human to another by haematophagous insects but that water can also help to spread.
miscellaneous
- Proteus morganii that causes fetid diarrhoea in children during the summer;
- Proteus vulgaris that causes diarrhoea, intestinal catarrh (a little like typhoid fever) and various infections;
- Listeria monocytogenes, responsible for listeriosis (blood, meninges, mucous membranes);
- Staphylococcus aureus, responsible for a number of skin or gastric disorders (abcesses, furonculosis, poisoning …) and is mainly looked for in swimming pool water;
- the legionella (whose main species is the Legionella pneumophila) that were found to constitute human pathogens in 1976 as the result of an epidemic affecting a number of elderly American Legion people (whence the name "legionnaire’s disease") who became contaminated by the air conditioning system in the hotel hosting their conference. In fact, the infections caused by these bacteria are of two types: an acute pneumopathy (legionellosis) or a more benign form (Pontiac fever). These germs tend to proliferate in hot water (air conditioning systems and air-cooling towers; domestic hot water systems; inadequately cleaned shower heads where deposits and, possibly, the presence of amoeba can encourage the presence and proliferation of legionella); they achieve optimum growth at temperatures of 35°C but this growth will be inhibited after 55 to 60°C. Contamination is usually airbone: the bacteria are spread by aerosols (air conditioned premises, Jacuzzis, showers …) and the mortality rate can rise as high as 10 to 25%;
- Leptospira (or Spirochaeta), especially L. icterohaemorragiae that causes Weill’s Disease (leptospirosis) which is very prevalent throughout the world. Mainly propagated in rodent urine (rats, coypu), the disease is contracted through bathing or ingestion; it sometimes affects sewer workers.
Alongside these well-known pathogens whose clinical effects have been the subject of much study, we need to include the opportunist germs that are capable of being virulent, especially in the case of those suffering from immunodepressant conditions. For instance, this will involve bacteria pertaining to following genuses: Yersinia (Y. enterocolitica: gastro-enteritis and diarrhoea), Aeromonas or Mycobacterium (especially "M. avium complex" or MAC, that is extremely resistant to chlorine and will infect lungs with symptoms similar to those of M. tuberculosis. M. tuberculosis).
Unlike the pathogens quoted above, these germs have the drawback of having adapted to the water environment. In particular, they can proliferate at temperatures close to 0°C in the presence of a dilute organic substrate and, therefore, in conditions similar to those found in a water main.
fungi
Pipelines may occasionally be infested by a microscopic fungus: Histoplasma capsulatum. This fungus is responsible for histoplasmosis.
We must not overlook the moniliases (caused by Candida albicans) that are sometimes contracted from swimming in the sea.
Excluding the above exceptional observations, there is no known waterborne epidemic caused by fungi.
the protozoa
Please refer to table 5 (animal kingdom) for the place of the following organisms in the classification system.
amoeba
As 10 to 15 µm diameter cysts, amoeba can survive in water for more than a month. However, they can be completely eliminated by means of an ozone treatment (CT of approximately 2 mg . min/L). Several waterborne species have important implications for human pathology:
- Entamoeba histolytica, a parasite in the strictest sense, responsible for amoebic dysentery which can sometimes be fatal (1934 Chicago epidemic);
- Naegleria gruberi, N. fowleri et Acanthamoeba polyphaga, "free" amoeba that are occasionally pathogenic in heated water: these amoeba are the cause of waterborne meningoenchephalitis, especially in swimming pools and cooling systems. These amoeba can also act as bacteria and virus reservoirs (e.g. Legionella).
flagellates
The main flagellate to remember in this category is the Diplomonadina Giardia lamblia (also known as G. intestinalis, G.duodenalis or even G. enterica), responsible for many gastro-enteritis ("giardiasis") and found in water throughout the world. Its dissemination is considerable due to the abundance of healthy carriers. It displays a high resistance to disinfectants, especially in its encysted form.
The ovoid cysts (figure 14) are from 8 to 16 µm long and 6 to 9 µm wide; they are fairly well eliminated by flocculation carried out at optimum treatment amounts followed by a rapid filtration through sand.

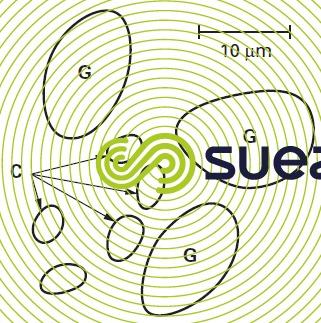

sporozoa
This division includes several "emergent" parasites, especially those pertaining to the order Coccidiae (Cryptosporidium,Cyclospora,Isospora,Toxoplasma) and whose encysted forms (oocystes) are particularly difficult to remove using conventional treatments; at present, these parasites are one of the factors driving the changes being made to drinking water treatment systems, particularly the development of ozone or UV disinfection processes (see Oxidation-disinfection) and, to a greater extent, filtration through MF or UF membranes (see Separation by membranes and Drinking water treatment).
- Cryptosporidium (C. parvum), responsible for cryptosporidiosis, has oocysts that are virtually spherical, having a diameter of 3 to 6 µm; they are noticeably smaller than Giardia cysts (figure 14). Many animal spacies (especially bovine, ovine and caprine) can act as reservoirs for this parasite. This disease has the same symptoms as giardiasis (diarrhoea, nausea and vomiting, abdominal cramps, headaches, fever); however, this parasite presents a particular danger to immunodepressed patients (babies, the elderly, AIDS patients). Chlorine is virtually powerless for eliminating this parasite; ozone works but at a concentration far higher that commonly accepted; the "multiple barrier" treatment, combining solid-liquid separation (including membranes if possible) and disinfection (O3 and/or UV) is alone capable of providing the consumer with an effective protection;
- Cyclospora (C. cayetanensis): spherical oocysts measuring 8 to 10 µm, that are infectious at the spore-forming stage (and, therefore, unlike Cryptosporidium, not immediately after their excretion). In this case, other mammals do not appear to act as reservoirs for this parasite. The disease has the same symptoms as cryptosporidiosis. As in the case of other Sporozoa, the oocysts are very chlorine-resistant;
- Toxoplasma (T. gondii): this parasite has a two-host cycle: a mammal (including Man) or a bird as the intermediate host and a carnivorous feline as the end host; it causes brain damage in babies and AIDS-related illnesses. Little is known at present about the effectiveness of treatments used to eliminate this organism;
- Microsporidia: this collective term applies to an order of Sporozoa that includes several pathogenic genuses: Enterocytozoon (E. bieneusi), Encephalitozoon (E. intestinalis), Nosema (genus also known as the insect parasite), Pleistophora, Trachipleistophora, Vittaforma, plus the "odds-and-ends" genus Microsporidium, that has yet to be clarified. These organisms form 1 to 5 µm long ovoid spores. The symptoms and the populations at risk are the same as for Cryptosporidium, but, apart from the use of membranes, less is known on the effectiveness of clarification-disinfection techniques on these spores.
worms
Parasitical worms hosted by Man or by animals belong to the helminth(from the Greek helmins = worm)group (super-division) and cause helminthiases; this group has two divisions (see also table 5 on metazoa section animal kingdom):
- Platyhelminths (or flat worms) that are also divided into two classes:
- Trematodes (e.g. bilharzia of schistosoma, liver flukes);
- Cestodes (e.g. Taenia, Hymenolepis);
- Nemathelminthes (or nematodes or roundworms) such as Ascaris, Toxocara, Trichuris (all three the most frequently detected in waste sludge and water), the eelworm, the hookworm, the dracunculiasis, the pinworm (bearing in mind that there are many free, non-parasitical nematodes (photo 5) in the soil, in surface and ground water and even in some media that are particularly rich in OM such as poorly maintained GAC filters or activated sludge).



Water can act as a carrier for most of them. These worms, their larvae and, above all, their eggs, are not destroyed by disinfection when used in normal amounts; however, due to their size (see below according to the different species), they are particularly well suited to clarification and, above all, to filtration: as a rule, they do not pose any problem in properly processed drinking water. Additionally, residual helminth egg levels are stringently regulated in UWW used for irrigation purposes. (< 1 egg · L–1, see Urban effluent).
Many of these parasitic worms continue their development in a series of a number of different hosts:
trematodes
Schistosoma cause a serious disease called bilharzisis or schistosomiasis, mainly widespread in hot regions of the Earth. There are two forms of the illness and three species of this parasitic worm:
- bladder bilharzia (or urinary bilharzias affecting the bladder) caused by the Schistosoma haematobium (Middle East, tropical Africa, Madagascar);
- intestinal bilharzia caused by S. mansoni (Egypt, tropical Africa, Madagascar, Latin America) or by S. japonicum (Far East).
The adult lives in human blood vessels. The egg is ovoid (50 × 150 µm) and has a 25 µm tip. It is excreted in urine and develops in water as a ciliated embryo (miracidium) that infects live snails in still water (bulinids, planorbids …). In the snail, it becomes a cercaria (forked tail larva) that is returned to the water and enters into a new human host through the skin (or the membranes of the mouth). A cercaria lives for approximately two or three days.
This epidemic is fought by destroying the intermediate host, i.e. molluscs: chemically (molluscicides) or biologically by altering the mollusc habitat.
In drinking water, cercaria can be eliminated by filtration through sand (max. ES = 0.35 mm in the absence of any coagulant); however and above all, the effectiveness of pre-chlorination and final disinfection (chlorine or ozone) will ensure that cercaria are destroyed provided appropriate amounts and contact times are applied (e.g. with chlorine: CT = 10 to 30 mg · min · L–1 depending on the species and on temperature).
Liver flukes are responsible for illnesses called distomatosis; we have the sheep liver fluke (Fasciola hepatica) and the lancet fluke (Dicrocoeliumlanceolatum); the adult worm is found in various locations but mainly in the liver in Man and in herbivores (especially sheep). As in the preceding case, the ovoid egg (70 to 130 µm) produces a miracidium in the water: this miracidium enters into the intermediate host, a mollusc (Lymnea in the case of the sheep liver fluke, planorbid in the case of the lancet fluke) where it proliferates as several larvae forms, resulting in the release of cercaria that become encysted (metacercaria) on an aquatic plant through which herbivorous vertebrates become contaminated (wild cress in the case of Man).
cestodes
Taenia solium (tapeworm): 35 µm spherical egg that forms a cyst in pigs.
Taenia saginata (beef tapeworm): 25 × 35 µm oval egg that forms cysts in beef cattle.
Diphyllobothrium latum [broadfish tapeworm] or Bothriocephalus latus [broad tapeworm]: adult in Man (in the small intestine, where it can grow up to 20 m long) who will then suffer from "bothriocephalic anaemia". The 45 × 70 µm oval egg develops in water, releasing an embryo that infects a copepod. The copepod is then swallowed by a fish and the embryo transforms into a 8 to 30 mm long larva that attaches itself to the muscles of the fish; Man is contaminated by eating insufficiently cooked fish.
nemathelminthes
Ascaris lumbricoides: frequently found in the small intestine in Man and in pigs. The adult worm is 10 to 20 cm long and lays 50 × 75 µm oval eggs. The egg develops in water or in damp soil, forming a 0.3 mm embryo that contaminates Man direct.
Oxyurus vermiculis: often found in children. 20 × 50 µm oval egg with one slightly flattened side. Does not appear to live for long in water.
Eustrongylus gigas: infects the urinary tract. Its 40 × 60 µm elliptical egg is lighter coloured at each end. The 0.25 mm long embryo infects fish as the intermediate host.
Ancylostoma duodenale(strongylus): a small 6 to 20 mm long worm that lives in the intestine, pierces the mucosa and causes extremely persistent haemorrhaging and diarrhoea (ankylostomiasis that can also be caused by a similar species, the Necatoramericanus). Its 30 × 60 µm egg develops in water where it requires a minimum temperature of 22°C. The 0.2 mm embryo produces a larva that is capable of passing through the skin to infect another host.
Filaria (or Dracunculus) medinensis(dragon worm, a worm found in Guinea, the Guinea worm). This is a viviparous animal. The 0.5 to 1 mm embryo infects a copepod (Cyclops) and forms a larva. This copepod is swallowed with water and allows the larva to develop in Man.
The worm crosses through the intestinal wall and forms sub-cutaneous abcesses (dracunculosis) that can develop into tetanus. Eliminating copepods through water treatment avoids any danger of contamination; however, contamination can occur if the larva passes straight through the skin.
Anguillula intestinalis: the 2 to 3 mm worm lives in the duodenum. The egg develops in water, forms a worm (Anguillulastercoralis) that lays its eggs in water and the ensuing larvae can recontaminate a human being who drinks the water or by crossing through his skin.
insects
Mosquitoes are the main aquatic insects that pose a danger to health; their larvae have to live in water and mosquitoes are responsible for transmitting certain diseases.
Malaria or swamp fever is transmitted by the Anopheles (A. maculipennis, funestus or gambiae), the Laveran hematozoa being responsible for spreading the disease. Yellow fever (typhus amaril) is transmitted by Aedes aegypti. The Culex genus can also carry certain diseases (virus encephalitis, Wucheria bancrofti).
Another filariasis, the onchocercosis (or river blindness transmitted by the Onchocercavolvulus), is transmitted by a small fly, the black fly whose larvae develop in fast-flowing rivers. The black fly also transmits a disease due to protozoa, leishmaniasis.
Bookmark tool
Click on the bookmark tool, highlight the last read paragraph to continue your reading later












